Blowing up a balloon
"There is a developing interest in impact of dysfunctional breathing in common conditions such as asthma, chronic back and neck pain, postural stability, cardiovascular disease, anxiety and depression" (Courtney., 2009, p.78). After completing both the myokinematic restoration and postural respiration courses with the Postural Restoration Institute, I was again brought back to the idea of retraining breathing patterns. These courses spend considerable time exploring breathing dysfunction, teaching clinicians how to objectively evaluate respiration and prescribing exercises that focus primarily on restoring the zone of apposition (ZOA). Prior to taking these courses I have always focussed on breathing technique with my patients and found that there will be a distinct lack of control and progress if patients cannot coordinate their breathing with movement.
When thinking about teaching breathing patterns two ideas come to mind:
- Breathe in through your nose, breathe out through your mouth making a haa sound as you exhale.
- Discourage pursed lip breathing, breath holding and/or hyperventilating.
This approach works for most people but when it doesn't I am not sure of the best approach to take for restoring normal breathing patterns. I was intrigued therefore to understand how I can further target breathing using the balloon technique.
Boyle, Olinick & Lewis (2010) discuss the potential missing link in core stabilisation programs, which they refer to as the zone of apposition (ZOA) and the coordination that exists between the diaphragm and abdominal wall. In this paper the authors refer to many of the significant papers published in the early 2000’s by researchers such as Richardson, Hodges and O’Sullivan around diaphragm and transversus abdominus (TrA) function/dysfunction in patients with lower back pain. This is the same body of evidence that I learnt from in Australia during my training about core stability, and, I do recall the emphasis that was placed on ensuring normal diaphragmatic breathing but it is only now in 2017 that I have been introduced to this term, the zone of apposition. One of the key aspects of restoring the ZOA is promoting exhalation.
"One of the most critical factors, often overlooked by physical therapists, is maintaining an optimal zone of apposition of the diaphragm. The zone of apposition (ZOA) is the area of the diaphragm encompassing the cylindrical portion (the part of the muscle shaped like a dome/umbrella) which corresponds to the portion directly apposed to the inner aspect of the lower rib cage. The ZOA is important because it is controlled by the abdominal muscles and directs diaphragmatic tension.” (Boyle, et al., 2010, p. 180)
90/90 bridge with blowing into a balloon. Image credit "Postural Restoration Institute" (used with permission).
How does it all work?
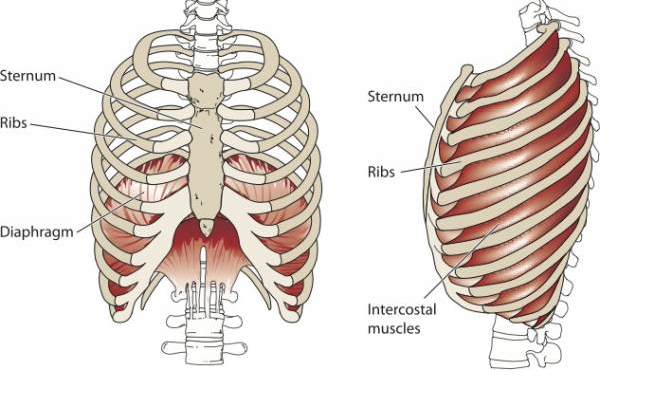
The ribcage and diaphragm. Image source: Google Images
Did you know that we breathe on average 21,000 times a day! Safe to say that our respiratory system has a large and continual functional demand that it has to maintain.
During inspiration the diaphragm will contract concentrically, move downwards and flatten out. This creates a negative pressure within the thorax and draws air into the lungs. At the same time the TrA contracts eccentrically. Yep, you're abdominal wall contracts and lengthens as we breathe. In a normally functioning diaphragm, inspiration will be accompanied by a forward displacement of the abdomen and a lifting and widening of the lower six ribs (Courtney, 2009).
During expiration the diaphragm contracts eccentrically along with the elastic recoil of the lung tissue to expel air from the lungs and the abdominal wall contracts concentrically. At the end of exhalation the lower ribs will draw down into the abdomen and this is where the zone of apposition is achieved.
So when we are considering the central point of core strength or core stability we have to begin by looking at how people breathe in and out during quite respiration and forced expiration. Asking someone to breathe in using their diaphragm doesn't necessarily mean they will do so.
One of the key ideas I took away from both PRI courses is that when breathing deeply we need to use all of the rib cage, not just the abdominal wall. If we just breathe into our neck and upper chest it is termed apical breathing. If we just breathe into the stomach and don't allow our chest to rise it is termed belly breathing. Another abnormal breathing pattern would be to suck in the stomach during inspiration. All of these come under the term paradoxical breathing. The ideal is to inhale and have the chest and stomach rise equally, thus using areas of the lungs equally too.
Some anatomical tips about the diaphragm (Boyle, et al., 2010):
- The anterior section of the diaphragm attaches to the xiphoid process of the sternum and ribs 7-12.
- The apex of the dome sits around the level of T8.
- The right half of the diaphragm attaches to the anterior part of the L3 vertebrae and the left half attaches to L1-L2.
- It's big and has a large surface area inside the chest.
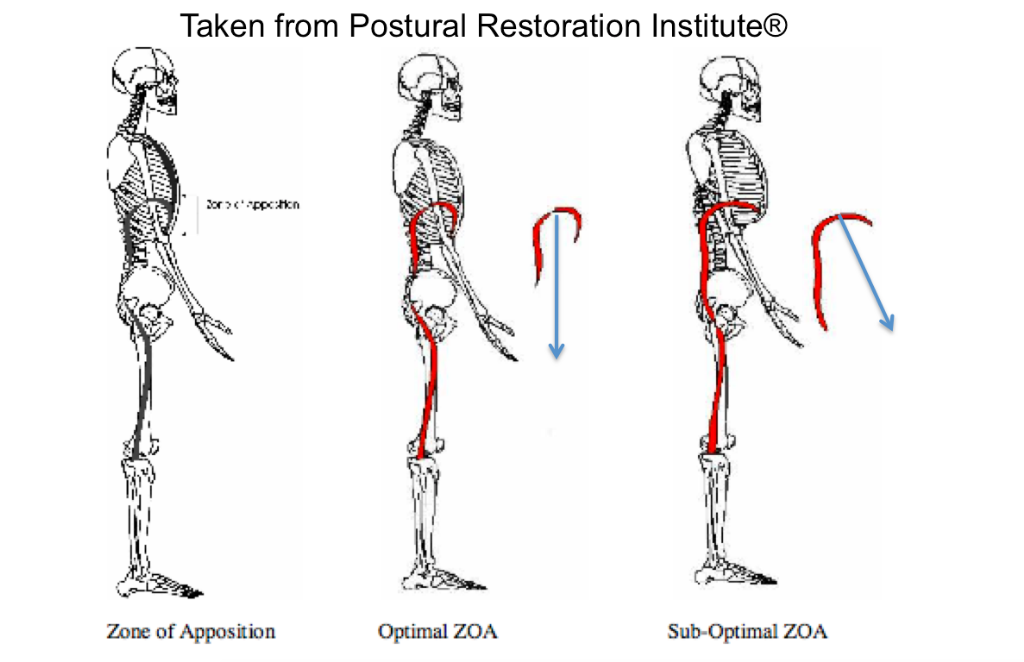
The zone of apposition (ZOA)
Some causes for loss of ZOA and paradoxical breathing include: hyperinflation and changes in lung volumes, abdominal weakness, ribcage stiffness, and altered respiratory drive from central mechanisms (Courtney, 2009). All of these factors will influence how the diaphragm functions and if the zone of apposition is achieved at the end of exhalation.
When the ZOA is lost the diaphragm can no longer draw air into the thorax optimally and often less air is inhaled. There is also less rib expansion, a compensatory increase in abdominal expansion and changes in the overall posture of the thorax. This can lead to a state of hyperventilation and hypocapnea and systemic impacts from excitation of the sympathetic nervous system. This includes alterations in blood levels of carbon dioxide, impaired nerve conduction, constriction of peripheral blood vessels, restriction in blood flow to the brain and heart, fatigue, weakness, peripheral neurological symptoms such as pins and needles, hypersensitivity to light and sound, and emotional responses such as catastrophic thinking, anxiety and panic attacks. Restoring and promoting normal breathing has widespread effects throughout the body.
Restoring the ZOA is achieved on expiration. To try restore the ZOA which is essentially a representation of optimal breathing mechanics, the Postural Restoration Institute developed an exercise known as the 90/90 bridge with exhalation into the balloon. The primary focus of this exercise is to optimise the ZOA and therefore is the foundation for all restoration programs.
Exhaling into a balloon
Here is a video of Ron Hruska from the Postural Restoration Institution teaching the 90-90 hip lift with balloon. This is one of their signiture rehabilitation exercises.
The reason the feet are placed on the wall at 90/90 is to promote posterior pelvic tilt, lumbar flexion and hamstring activity. Due to the line of pull of the hamstrings and their attachment on the pelvis, they act to pull the lumbar spine into flexion during the exercise. The aim of this is to inhibit extensor paraspinal activity which could interfere with diaphragmatic and abdominal control. A 4-6 inch ball is placed between the knees to encourage adductor tone which co-contracts with the pelvic floor muscles.
The patient is directed to hold the balloon in their mouth and breathe in through their nose while resting their tongue on the roof of their mouth. The inhalation is to about about 75% maximus volume over 3-4 seconds. Then the patient exhales for 5-8 seconds and pauses for 2-3 seconds at the end of exhalation.
After the first breath the exercise becomes more complicated. For the second breath in, try to inhale through your nose without pinching the neck of the balloon with your teeth, lips or fingertips. If you can’t achieve this, it is an indication that you are unable to maintain intra-abdominal pressure during inspiration without the air from the balloon coming back into your mouth. The ribs are held down during the second inspiration which directs the air into the apical regions and posterior regions of the lung. This kind of inspiration encourages further rib rotation during inspiration and feels great if you suffer from stiffness through your upper back. Often the upper chest expansion can be restricted by tight soft tissue structures such as subclavius or pectoralis minor and pectoralis major. In order to breathe apically, these soft tissue structures around the shoulder girdle need to relax and lengthen.
A good test to see if someone is able to expand the posterior aspect of their chest sufficiently during inspiration is with accompanied anterior chest/mediastinum compression. PRI uses inspiration in standing forward flexion and I’ve always used child’s pose position with arms by the side. Biomechanically they achieve the same thing in the thorax i.e. they provide a block to movement at the front of the chest and encourage posterior chest expansion, but each position has a different postural demand, balance requirements, and different amount of hamstring mobility.
"The BBE is a specific example of an exercise that could be useful for integrating co-activation of deep abdominal muscles with pelvic floor and diaphragm during neuromuscular training and a wide variety of stabilizing manoeuvres.” (Boyle, et al., 2010, p.186) Clinically, it is a useful objective tool to help us determine if our patients are breathing correctly in a resting position. If you'd like to learn more about this concept I would recommend reading the reference below and consider taking the online courses hosted through PRI. The other benefit of these courses is that if this exercise is ineffective in restoring the ZOA (and the assessment for this is covered in the course too), then PRI teaches many manual techniques targeting thoracic and rib mobility.
Integrating ZOA with abdominal exercises
Below is a video of Jill (a former colleague and incredible Pilates Instructor) teaching me how to perform a abdominal curl without overusing my hip flexors and focussing on breathing control. What you'll notice is that Jill, who isn't PRI trained, uses the same approach with breathing to optimize the ZOA, keep the ribs tucked into the abdominal wall and promote breathing into the back of the rib cage. It's always exciting to see common ideas across different professional domains. Regardless of whether you use a balloon, call it the ZOA, or just talk patients through breathing control, the common theme is breathing well to promote optimal motor control and coordination.
So the question is - do you know how to breathe?
Sian
References
Boyle, K. L. (2010). The Value of blowing up a Balloon. NAJSPT. North American Journal of Sports Physical Therapy| Volume, 5(3), 179.
Courtney, R. (2009). The functions of breathing and its dysfunctions and their relationship to breathing therapy. International Journal of Osteopathic Medicine, 12(3), 78-85.