Hacking into your own rehab
This is a first for Rayner & Smale, which I hope paves the way for future discussions about optimising patient recovery, and involves a open dialogue between myself and my client Sophie. The idea stems from my continual drive to ensure that patients feel engaged in their own rehabilitation and empowered to drive their own journey. But more than that, they need to know how and they need to want to do it. I once heard a phase from a Physio I greatly admire as he spoke to his patient about being actively involved in the recovery process:
I can see the journey you are going to embark on and I will sit beside you as we look out in the same direction, but I will not sit in the front seat and drive you there.
That phase has implanted itself in my motivation to helps others tap into their rehab potential. Occasionally I might repeat it, but more than often it has lead me to ask my patients the following questions:
- What has and has not worked for you in the past?
- What do you want to be able to do?
- Can you can help me identify your goals for recovery? From there I will work out the problems and together we will work out the best way for you to achieve them.
Building trust
When I meet a patient for the first time, more often than not the main goal for the first session is to get to know them and try establish a level of trust. They need to understand what I can offer and trust me enough to produce the outcomes. Otherwise they won't return.
Working in San Francisco has demanded me to change some of the ways I practice and communicate with my patients. I've needed to become more accessible and reachable via email, even if it means some after-hours or weekend conversations. Instead of only talking during consult time, when needed, we can email back and forth. Most patients want to feel like they can independently solve their own problems and their work schedule often dictates how frequently they can attend, especially when they travel in and out of the city. As such, they need to be super accountable for their own rehab and for this I use Google spreadsheets (and filming patients do their exercises on their phones). A spreadsheet is not fancy, but it is free and easy to use and certainly beats my infamous stick figure drawings.
Understanding what drives you.
During the first appointment with Sophie, I recall asking her what her previous experience with physiotherapy had been. Sophie loved her previous Physiotherapist, but since moving to San Francisco, had not found the same connection and trust with several different PTs. Sophie, like me, is from Australia and this definitely helped in building rapport but what struck me more was that Sophie was incredibly upfront with what her experience and expectations were about Physiotherapy. She admitted to slacking in the area of compliance towards home exercise programs, wanted a therapist that would push her, make her as independent as possible and be able to come only when is needed, rather than on a regular review. Fine by me (I thought) but you'll have to do the work and no slacking! Sophie and I have a very open rapport, we are upfront and honest about what we both think (which I love so much) so I thought she'd be a great patient to discuss compliance and motivation for change with. When I asked Sophie if she would share her experiences to date with me for this blog, these were her thoughts (in italics).
I’ve been a patient of various physios since I was a child (stress fracture, torn ligament in my foot, three sprained ankles, sports-related shoulder spasms, ITB strains, hip tear) and my biggest issue has always been actually doing my physio homework. Usually I would follow their advice religiously until my life wasn’t particularly impeded anymore i.e until I could play Saturday netball, go for a run, walk without pain; rather than continuing to rehab until I was fully functional again.
After that I would:
- Forget what my physio told me to do,
- Lose the bit of paper on which I scribbled down the exercise descriptions; and
- Feel reluctant to fork out cash for my physio to tell me to keep doing what I had been doing.
Earlier this year I had a skiing accident, landing a serious bone bruise and a partial ACL tear. Sian’s approach to managing my rehab has felt revolutionary due to two factors:
- Systematic: Her use of google docs to keep me accountable
- Emotional: Her attitude and goal setting approach to keep me motivated
Be systematic. It is not a cake recipe.
I know this sounds a little cheap but I don't believe in recipe treatments and I don't offer them to patients. I believe that everyone needs to be assessed individually and provided with a tailored program. Using Google Spreadsheets allows a dynamic outline of rehab goals and progression of exercises. It is a systematic way to help patient's understand their problem and goal lists. Not everyone needs a spreedsheet, some prefer emails, some love paper, but Sophie has used it so well and it has made our sessions feel like an effortless continual discussion even when 3 weeks apart.
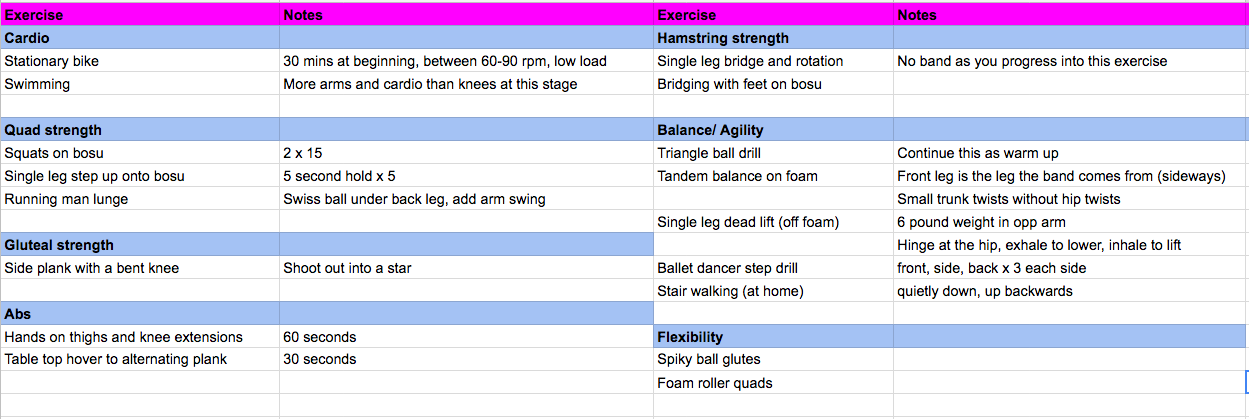
Sian created a rehab spreadsheet for me on google docs, which took her about 5 minutes. She grouped my exercises under headings like “Cardio”, “Gluteal strength”, “Balance/Agility” and noted descriptions next to them like “Remember: knee control and bum muscles” – words that actually mean something to me.
I downloaded the google sheets app (which is free) so that I always have it with me at the gym. I then enter the date of my workout on the top row. I enter in the notes as I’m wiping down the gym bike “Felt bit clicky. No pain. ITB tight.” Same thing on my other exercises: “Only did 2 sets. Glutes too fatigued for 3rd” or “Need to be reminded how to do this one.” It takes me no time at all. I don’t write notes for every exercise – just if there’s something that feels relevant to my recovery.
Not only does this make me accountable because Sian can see how many sessions I did between our appointments, it actually make me feel like we are creating my program together.
When I come in to my appointment Sian has all of my notes on her laptop and I don’t have to rack my brain when she asks me if my left glute felt stronger than my right during my bosu squats – it’s all in the notes! Sian creates a new sheet each time she adjusts my program and spends the last few minutes of our appointments typing in the descriptions in front of me, using language I will remember (“Sian, call it the ballet dancer step drill”).
Session 8 review plan
Emotional support & identifying the priorities.
Sophie has a partial ACL tear and massive bone contusion. Her main goals at the moment are to allow for the bone bruise to heal, while making the most of this time to develop amazing dynamic balance and rotational control around the knee. Here are some of her exercises.
More than the physical elements of improving her range of movement, strength, dynamic balance and rotational control, Sophie needs encouragement and support. It takes months to recovery from a bone bruise and it takes courage to rehabilitate a partial ACL tear that currently does not warrant surgery, yet is not as functionally as stable as a normal ACL. Sophie needed to have steps in place to regain control over her life, optimise her exercise routine for her stage of recovery, and identify the steps that were required to successfully rehabiltate this challenging injury.
Even though I’ve had my fair share of injuries over my life, none have been as debilitating as my current one. The story is common: athlete (or in my case, semi fit person) injuries herself, is out of action for 6 months, gets frustrated, focuses attention on the activities she can’t do, loses perspective of the potential recovery period, tries not to whine about it buts hits breaking point when she tries to carry two bags of groceries up the two flights of stairs to her apartment in the annoyingly hilly city of San Francisco. That last bit might be anecdotal but all physios would recognize the rest.
I’m not sure if physios are taught this or whether Sian is just super in tune with people (the latter is definitely true) but Sian takes the approach that physios are not just treating an injury – they are treating a person whose attitude to their injury is going to determine the length and quality of their recovery.
When I came to Sian I had an incorrect diagnosis, I’d been in pain and unable to walk for 6 weeks and I spent 40% of my daily attention span thinking about things like whether I could ever play tennis again without fear of snapping my ACL. Basically, I had the wrong attitude for recovery. Here is a list of things Sian did to get me out of my head:
- Set specific 6 week goals with me (“I want to be able to walk 6 blocks without limping”)
- Always made me focus on the movements I could do and developed a rehab program around them.
- Was generally really encouraging and validated my progress.
- Made me focus on the non-exercise related things that I could do for fun / stress release.
- Incorporated exercises into my rehab program based on my unique goals (“When you can show me that you can safely do exercises a,b,c, you can try a yoga class”).
In summary, the google docs idea is super easy to implement and makes a world difference and an encouraging coach-like approach from my physio has made it far easier for me to just get on with life.
I have to admit, I was surprised by Sophie's response to my question because I hadn't full realised how something so simple as a spreadsheet could make such a difference. Sometimes the most complex part of getting better is finding out what needs to change for recovery to occur. Identify the barriers, recognise our strengths and weaknesses as much as our patient's. Set goals and be accountable for reviewing them. And remember that knowledge is empowering! If we can learn about Physical Therapy, there is no reason why our patient's can't learn to be their own therapists as well.
I will sit beside you as we look out in the same direction, but I will not sit in the front seat and drive you there.
Sian & Sophie