Introducing the Imprecision Hypothesis in Chronic Pain
On September 26th & 27th 2015 I attended the Californian Annual Physical Therapy Conference in Pasadena, California. What a mind blowing weekend. Lorimer Moseley was the Keynote Speaker and I loved listening to his lectures. It never seems to stop… the learning, the questions and the sharing of ideas. Continuing education and learning is an ingrained and integral part of my being and professional identity and I love going to places and without expecting it, having my understanding and knowledge challenged and changed. How lucky are we to be surrounded by such great minds.
It’s hard to capture everything I learnt so instead I’m going to share with you some of the key ways my thinking changed or developed. Before attending the conference I didn't know:
- What associative learning of pain meant.
- What the Imprecision Hypothesis was.
What is the imprecision hypothesis?
The Imprecision Hypothesis is not Central Sensitisation but a hypothesis that aims to explain how aspects of chronic pain may occur. Central sensitisation involves non-associative mechanism where non-noxious stimuli come to manifest as allodynia, hyperalgesia and spreading of receptive fields. The Imprecision Hypothesis presents pain as a conditioned response to the multi-sensory and meaningful events that routinely coincide with, or prompt, nociceptive input (Moseley & Vlaeyen, 2015, p.37).
In 2015 Moseley & Vlaeyen published a paper in Pain Journal titled “Beyond Nociception: the imprecision hypothesis of chronic pain”. Both the original paper and reply to letter to the Editor are available through the Body In Mind website (a great resource for learning about current concepts in pain science). This was the first I had heard of this new hypothesis, which aims to explain the origins of chronic pain in a variety of common pain disorders such as widespread chronic pain, non-specific back and neck pain, and fibromyalgia. Previously I have written about central sensitisation and the pain neuromatrix, concepts that have helped me understand the complexities of chronic pain disorders.
The Imprecision Hypothesis is independent yet linked to the theory of Central Sensitisation and helps provide a possible explanation as to why chronic pain occurs.
"We still do not know why chronic pain develops in some people and not in others …. and it seems that despite extensive advances in multiple fields, we have made little ground” (Moseley & Vlaeyen, 2015, p. 35).
So where did this idea arise from?
The reason it was developed is that central sensitisation doesn’t fully explain deficits common in chronic pain such as changes in tactile acuity, dysfunction in memory and executive functioning, and widespread nonspecific body pains. Hence these authors and scientists have been searching for more answers. “A very large body of evidence demonstrates that nociception is neither sufficient or necessary for pain” (Moseley & Vlaeyen, 2015, p. 35).
The imprecision hypothesis relates to associative learning of pain, meaning that pain is a response not a stimulus, and that specific encoding of nociceptive input relating to painful events results in us learning and encoding information that is then generalised to similar future events. Pain is a conscious experience that can be and often is associated with nociceptive input but relies heavy on neurobiological, environmental and cognitive events (Moseley & Vlaeyen, 2015). The encoding of nociceptive inputs is almost always coupled with other multi-sensory events.
We have known for some time now that plasticity in the neural networks plays an important role in the development of chronic pain.
- Plasticity can occur in a non associative ways which explains habituation and sensitisation from repeated exposure to a stimulus (central sensitisation features).
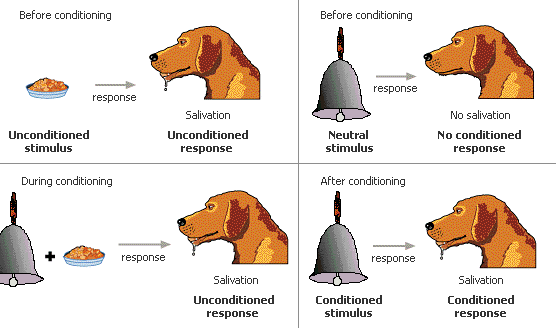
- Plasticity can also occur in an associative way and the example we were all taught about associative learning is Pavlov's dog and the conditioning of the bell with salivation….. hopefully I don’t need to repeat that story but here is a picture to help jolt your memory.
Pavlovian dog experiment which demonstrates the pairing of a unconditioned stimulus to a conditioned stimulus with the unconditioned response and the outcome being a conditioned response occurs (http://www.mywoofgang.com/images/PavlovDogWithBell.GIF)
Associative learning in pain
- Pain is considered the unconditioned stimulus.
- Fear is considered the unconditioned response.
When pain is paired with an unrelated conditioned stimulus that stimulus then elicits the same response as pain and is now referred to as a conditioned response. From here future situations can elicit fear prior to pain and avoidance behaviours occur in response to that fear. "We propose to extend this associative learning framework of pain-related fear to an approach that has pain itself as the response, rather than the stimulus” (Moseley & Vlaeyen, 2015, p. 35).
"The more “blurred” the encoding, the more generalization occurs and the more likely it becomes that pain will be triggered by more functionally distinct stimuli. That is, imprecise encoding of the original painful event, which may be, for example, bending forward, results in generalization of back pain to similar movements and activities. This mechanism actually offers a biological advantage because it affords a buffer of protection. However, at some point of generalization, the protective function moves from being adaptive or helpful to being maladaptive or unhelpful” (Moseley & Vlaeyen, 2015, p. 36).
A reply to a Letter to the Editor was released in 2015 which helps clarify some of the confusion that has arisen from trying to understand this new hypothesis and there is one section which I wanted to include in this blog as I think it clearly describes this hypothesis. ... The Imprecision Hypothesis is a 'fundamentally different conceptualization of pain: that of a perceptual inference that motivates protective behavior, rather than serving as a readout of nociceptive input or tissue dysfunction... We actually propose imprecise encoding of the conditioned stimuli (not conditioned response)' (Moseley & Vlaeyen, 2015, p. 2109).
It differs from central sensitisation which is based on non-associative mechanisms for example allodynia occurs when a non-noxious stimulus elicits a painful response. Allodynia, hyperalgesia and spreading of receptor fields is known to occur in central sensitisation but this differs from the imprecision hypothesis which suggests that associative learning occurs from imprecise encoding of a noxious stimulus with a multi-sensory event that then leads to the conditioned response of pain when that multi-sensory event is activated by other sensory messages (maybe visual cues).
Central sensitisation and associative learning are not mutually exclusive in the manifestation of chronic pain (Moseley & Vlaeyen, 2015).
Image left: a visual diagram of precise and imprecise encoding in the Imprecision hypothesis (Moseley & Vlaeyen, 2015, p. 36)
Image right: a visual representation of associative learning of pain (Moseley & Vlaeyen, 2015, p. 36)
How does this relate to clinical practice?
An interesting learning point is that if this encoding is multi-sensory then therapists need to be mindful of the precision of our pain education and how this may influence that encoding.
The brain is no longer viewed as a pain neuromatrix with 9 common areas of the brain active in relation to pain. Instead scientists are now realising that although there are 9 more commonly involved regions, there is actually a vast array of neuro-immune networks within the brain and these are referred to as neurotags. For pain to occur and series of neurotags need to be activated and those neurotags are strengthened and reinforced through repetition. So we need to be careful to repeat the correct things and strengthen the helpful and healing neurotags. Single neurotags activated alone don’t result in pain and every neurotag is a multi-tasker. Ultimately it is all about influence which means the number of neurotags involved and the precision of the activation pattern is essential to the output generated. The more you work a neurotag the more precise it becomes. What this means is that the terms pain processing and pain neuromatrix may soon be changed because we now know that these neurotags are not just functional in pain but in fact multitasking neurotags.
In regards to clinical practice, very important point that I took away from the conference is be precise about the words we use to describe what we know about the neurobiology of pain. This is very important and even I am at fault of making this mistake. If the neurotags in the brain relating to pain are extremely sensitive to thought processes and beliefs, then we need to do our very best to choose the right words and activate the right neurotags.
There is an input into the brain - the brain decides what the meaning is - and the output is created. Therefore the input…. which includes words… is critical to influencing the output. In chronic pain there is an increase in neuronal mass and an imprecise representation of the danger message with our pain neurotags getting really good at being activated and amplified.
Nonsense terms: pain receptor, pain pathway, pain fibres, pain message, pain signal and pain stimulus. None of these exist.
Sensible terms: Nociceptor, spinal nociceptor, nociceptive pathway, nociceptive message or signal, noxious stimulus.
I definitely have used these terms before in my blogs and would now like to use my new knowledge to better educate my audience.
So please start using these terms….
Friendly and accurate terms: danger detector, danger transmitter, danger messenger, danger nerve, danger message, potentially dangerous stimulus.
Q: Why should we change our language to reflect these terms?
A: Because we know now and strongly believe that pain is about protection and not damage.
The Imprecision Hypothesis proposes that faulty imprecise encoding of danger messages is involved in the development of chronic pain and therefore to successful treat chronic pain we need to restore the precision of coding of messages. This involves a variety of stages which depend on the severity of the condition. We need to start by focusing on the cortical body matrix which means addressing how our brain perceives reality and the picture is has of our body. Reality and perception are fundamentally linked and therefore we first need to alter our perceptions.
- We need to improve tactile acuity, sense of ownership over body, and reinstate precise intra-cortical inhibition in the pre-frontal cortex because the pre-frontal cortex plays a vital role in telling the neurotags to get ready and telling others (unwanted neurotags) to keep quite.
- Graded Motor Imagery
- Mirror box therapy
- Then we need to find the flare up line and change the buffer zone between the pain protection line and tissue tolerance line.
- Precise representation relies on accurate inhibition and therefore we can’t keep going beyond the flare up line. You need to activate the correct neurotags without initiating the undesired response i.e pain.
- Once the flare up line has been found then graded re-exposure to activity is needed (without triggering the undesired response) to retrain the brains inhibitory mechanisms and help make the encoding of danger messages and other multi-sensory events more precise.
In conclusion...
The Imprecision Hypothesis aims to explain how imprecise encoding of multi-sensory events coupled with a danger message leads to overgeneralisation of a response (in this case pain) and why protective mechanisms can change and become maladaptive mechanisms which are distressing and disability (Moseley & Vlaeyen, 2015). Although the Imprecision Hypothesis is yet to be proven, there is a large body of knowledge that shows that it is biologically plausible and it is testable. The Pavlovian theory of associative learning has been well supported by the literature which gives this hypothesis depth and strength and hopefully future research will provide further insight into it’s involvement in chronic pain. There is also a strong link to this hypothesis and the clinical development of imprecise cortical representation of body image, which is where graded motor imagery and mirror box therapy come into play.
The Imprecision Hypothesis is a new framework and still in the experimental phases. What we do know is that in chronic pain our capacity for precise representation is lost because our descending inhibition becomes faulty, and this theory helps to explain this. Personally, I find these new ideas and developments in knowledge to be exciting as we continue to push to know more about pain. What it does suggest is that maybe we have to work harder in the acute phases of pain not to distract and provide analgesia but to ensure that precise encoding of the painful event occurs. What a shift this will be….
Thanks for reading and I hope this has helped clarify your understanding of the mechanisms of chronic pain and introduce the most current literature and also point out where change is needed in the things we say. I have learnt so much from this conference and where my explanation of pain and sharing of knowledge can become more precise.
Sian ;)
Resources:
Moseley, G. L., & Vlaeyen, J. W. (2015). Beyond nociception: the imprecision hypothesis of chronic pain. Pain, 156(1), 35-38.
Moseley, G. Lorimer; Vlaeyen, Johan (2015) Response to the Imprecision Hypothesis Pain 156(10) 2019-2101
If you’d like to read about this approach to treating chronic pain I would recommend the article by Moseley & Vlaeyen, the resource the Explain Pain Handbook and also read my previously published blog explaining DiMs, SiMs and the Protectometer using a clinical example.
I’ve previously shared a clinical case study about fear-avoidance and kinesiophobia behaviour and it becomes clearer now how the Imprecision Hypothesis fits into that story.