Turning down TFL
One of my previous blogs focussed on the specifics of performing a lunge and other functional exercises to promote optimal gluteal activation. It focussed also on reducing TFL activity compared to gluteal activity, but did not provide any strategies for managing TFL itself. Recently I asked a group of physiotherapists the question "What are your tips for reducing TFL overactivity?" There was a general consensus that specificity of technique is the most crucial part of promoting gluteal activation over TFL.
When I started researching the topic of tensor fascia lata (TFL) overactivity & overload I was surprised by the limited amount of high-quality research on this topic. Perhaps this is a reflection of the problem itself and my guess is that TFL tendinopathy or overload issues are normally secondary to gluteal dysfunction or hip joint pathology.
There is however, a large body of research developing around the role of the kinetic chain muscular control in the presence of lower limb and back injuries. With patellofemoral joint pain in particular, weakness in the hip muscles which control dynamic knee valgus and femoral internal rotation have been associated with abnormal loading of the joint. Some inferences can be made from the outcome of studies on these conditions about the importance of lower limb alignment, muscle control and the correct performance of the kinetic chain.
The aim of this blog is to briefly discuss why TFL becomes overactive, review some of the literature behind minimising TFL activity and then to share some addition clinical tips that I use to progress rehabilitation.
Why is TFL overactive?
This is the most important question to ask.
TFL is a small ribbon-like muscle (about 18cm in length) which originates from the external iliac crest between the anterior superior iliac spine and iliac tubercle, and runs inferior-laterally to insert into the proximal iliotibial band (ITB) at the level of the greater tuberosity (Boss & Connell, 2002). The function of TFL is as a secondary hip flexor, abductor and internal rotator. It exerts force on the hip directly and indirectly on the knee through its insertion into the ITB (Cleland, 2005, p.250).
So the first possible answer is that there is muscular weakness in primary hip flexors, abductors and internal rotators. Sutter and collegues (2013) reported that TFL is often found to be hypertrophied on MRI investigation of patients with tears present in gluteus medius and minimus. This finding reinforces the concept that overload of secondary muscles exists in the presence of dysfunctional/deficient primary muscles.
Muscles of the anterior hip and thigh (Cleland, 2005, p. 251)
What are the other muscles producing similar actions to TFL?
Hip flexion is controlled by psoas major & minor, iliacus, and rectus femoris. When retraining hip flexion movements you may need to focus cues on activating these muscles. This may include drawing the hip back into the socket and feeling a activation through the front of the hip. Also watch for slight tricks and deviations through rotation as the hip flexes. As you can see in this picture, TFL lies laterally to the line of pure hip flexion and therefore patients might trick into internal hip rotation and then flexion which would bring TFL into a good line of force production. Keeping the hip in neutral rotation will hopefully avoid over activating TFL. If that movement isn't pure, then start in sitting with an isometric hip flexion contraction bringing the knee into the hand and making sure the movement stays in the sagittal plane.
Hip abduction is controlled mostly by gluteus maximus, gluteus medius and gluteus minimus. Tips for correction for hip abduction include:
- Placing hands over the buttock to palpate the muscles posterior to the greater trochanter,
- Starting in relative abduction by placing a pillow between the knees,
- Aiming to keep the ankle horizontal and avoid internal rotation,
- Kick the leg towards 11:30 for a bit more hip extension & avoid forward deviation into the coronal plane,
- Keeping the trunk still with a small gap under the bottom side on the floor to reduce a trunk lateral flexion substitute movement,
- Reaching long through the entire leg and lengthening out of the hip socket, and
- Minimise lumbar extension by starting with neutral pelvic position.
Deep muscles of the buttock (Cleland, 2005, p. 249)
Hip internal rotation is controlled concentrically by gluteus medius and minimus, TFL, and assisted by pectineus and gracilis.
Hip external rotators will eccentrically control internal rotation. The hip external rotators include gluteus maximus, superior and inferior gamelli, obturator externus & internus, piriformis and quadratus femoris.
So many muscles to consider and they all need to work in synergy to produce the desired movements around the hip and centre the femoral head for stability at the hip.
A little clinical anatomy...
TFL is innervated by the superior gluteal nerve (L4, L5, S1) and so are gluteus medius and minimus. Therefore when understanding why TFL is behaving it the way it is you may need to look at the function of contributing lumbar spine levels and also the other muscles innervated by the superior gluteal nerve. Gluteus maximus is innervated by the inferior gluteal nerve. (Cleland, 2005, p. 248-250).
Why is gluteus maximus function so important at the hip and knee?
It has reported that Glut max has a very large tendinous insertion into the upper aspect of the iliotibial band, which explains the control that glut max and the thoracolumbar fascia can exert on the knee (Antonio, et al., 2013). And if we continue to look higher up the kinetic chain into the lumbar spine, do Carmo Carvalhais et al (2013) found that active tensioning of latissimus dorsi impacts the contralateral hip's resting position through myofascial force transmission, and causes the hip to rest in a more externally rotated position. The fascial connection of Latissimus Dorsi to Gluteus Maximus through the thoracodorsal fascia is just another consideration that needs to be made when hypothesising the contributing factors to TFL overload. In summary, Lat dorsi strength and glut max strength both have a impact on hip joint position and control. As Maitland would teach us, assess the local structures at the site of pain, the structures which refer to it, and the joints above and below.
What does it look like if TFL is overactive?
Interestingly, in patients with advance hip joint osteoarthritis, the lower portions of gluteus maximus atrophy, while TFL and upper gluteus maximus remain the same size, and there is increased bulk through upper portions of vastus lateralis, when assessed with MRI (Grimaldi, et al., 2009). But the results of this study cannot be extrapolated to all types of hip and groin pathology. Patients with anterior groin pain have been found to display significant increases in AP diameter of TFL and hypoecogenic cone-shaped area in the tendon close to the insertion on the iliac crest, when assessed with ultrasound imaging (Boss & Connell, 2002). And patients with gluteal tears have been found to present with hypertrophy in the TFL on the affected leg (Sutter, et al., 2013).
Functionally, patients may present with a strategy to use femoral internal rotation and a medial knee displacement with movements such as sit to stand, step ups and walking/running.
Exercises to reduce TFL overactivity?
Enough about anatomy and function. Let's look at some exercises.
"If the goal of rehabilitation is to preferentially activate the gluteal muscles while minimizing TFL activation, then the clam, sidestep, unilateral bridge, and both quadruped hip extension exercises would appear to be the most appropriate" (Selkoitz, Beneck, & Powers., 2013, p. 54). Sidorkewicz, Cambridge, & McGill (2014) asked a similar question about muscle function when comparing clams to side lying abduction and their results favoured the clam over abduction for maximal gluteus medius activation. Clinically, I'm careful with going straight to clams based purely on this data because if there is any element of gluteal tendinopathy, the clam is going to compress and likely aggravate the tendon, and in that case, abduction is better. If you're starting with abduction (which is fantastic for glut max control), vary the degree of hip rotation from neutral to internal to external to see what works best for your client. Lee et al (2014) suggest that slight internal hip rotation will actually reduce TFL activity and promote more gluteus maximus and medius. As you read earlier though, my preference clinically is to maintain neutral hip rotation and work on cueing for better gluteal activation. The pictures below represent gluteal exercises where TFL is not preferentially activated (still active but not dominant).






But we can't just limit clients to these few exercises and we need tips for reducing TFL overactivity in other exercises and planes of movement too.
In a weight bearing (closed-chain) position tips for correction include:
- Drawing weight back into the heels.
- Imaging drawing the femurs back into the hip sockets to reduce quad bulking/bunching at the front.
- Weight bear more through the medial heel and then rotation the knee outwards from the hip to engage the gluteals.
- If indicated, posterior pelvic tilt in standing to reduce the amount of standing hip flexion, anterior pelvic tilt and lumbar lordosis.
Lengthening out of the legs and through the entire body.
All of the exercises above are great for strengthening gluteals with minimal TFL activity, but I also like these two demonstrating theraband external rotation strengthening. I love this exercise for training a more pure hip rotation movement and isolating the deep hip rotators. It feels so different to a clam because its not bringing in glutes as much. Aim to feel a contraction in the middle of the buttock behind the greater trochanter. Tips for correction may be to imagine pushing the knee backwards (to centre the femoral head) and activating pelvic floor (it has deep connections to deep hip rotators) to enhance muscular activation prior to the movement beginning. Avoid lifting the foot and activating hamstrings. Progress into 2PK.
On the reformer you can use the same cues and tips to do a sequence of leg strengthening exercises. What I try focus on is training correct posture and making sure the client feels the right muscles working (gluteals, VMO, calves etc... not TFL).
- Double leg press with a focus on driving through the heel and lengthening out of the hip sockets.
- Double leg press with toes on bar and then turn out focusing on foot posture and hip external rotation.
- Single leg press in side lying driving through the heel and maintaining external rotation at the knee.
- Side lying legs in straps both single leg press and abduction focusing on hip and knee positioning in space.
- Supine feet on bar and practicing hip external and internal rotation without TFL catching and overactivity.
- Supine bridge in parallel or turnout with or without leg press.
Tips for correction on the reformers:
- Lengthen the leg out of the socket in extension.
- Maintain neutral spine - no flaring of ribs, no height difference from ribs to anterior pelvis, no upslope into hips, no flat back
Using foot posture through 1st met and then external rotation from hips to get deep hip external rotators.
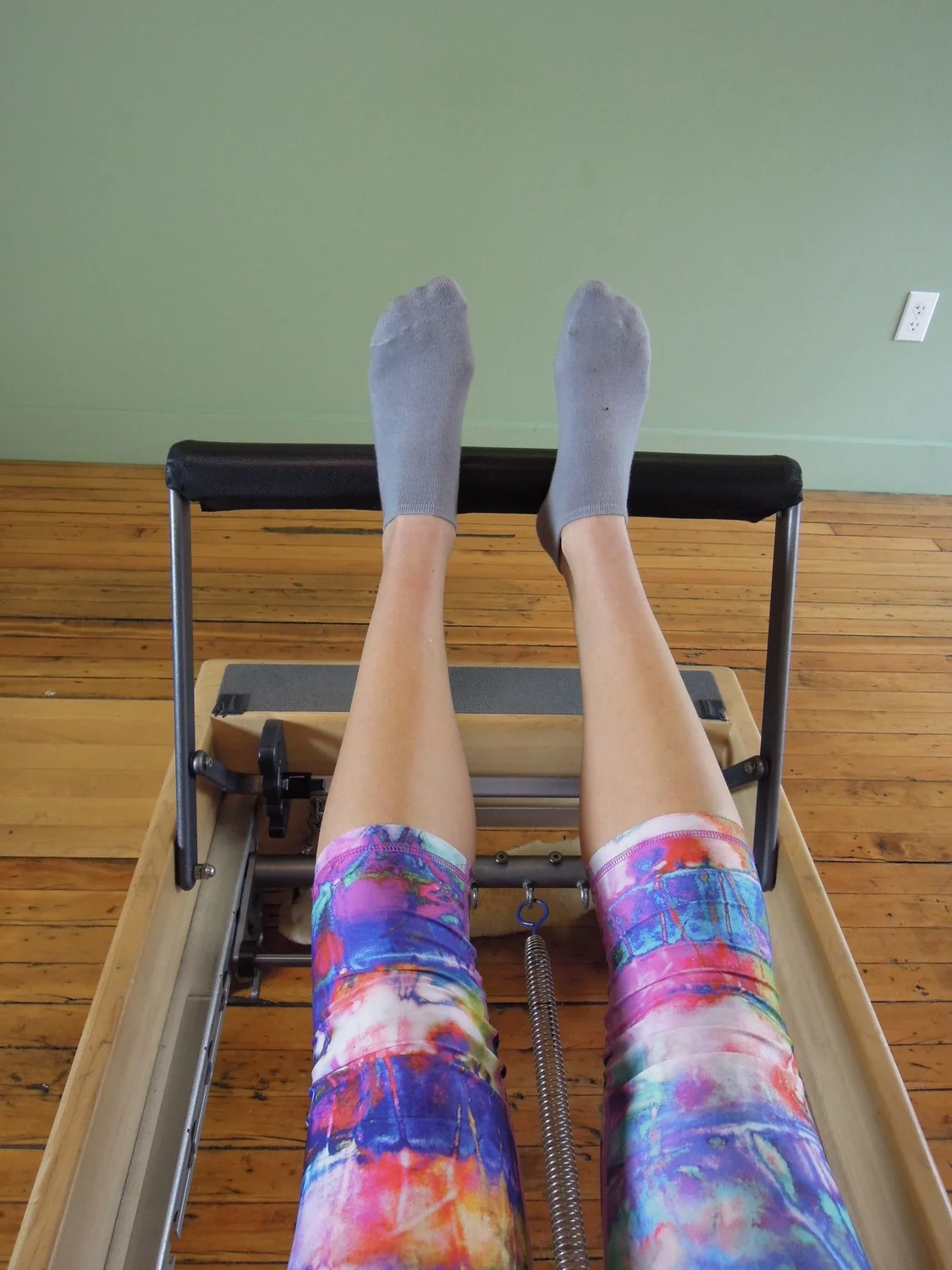





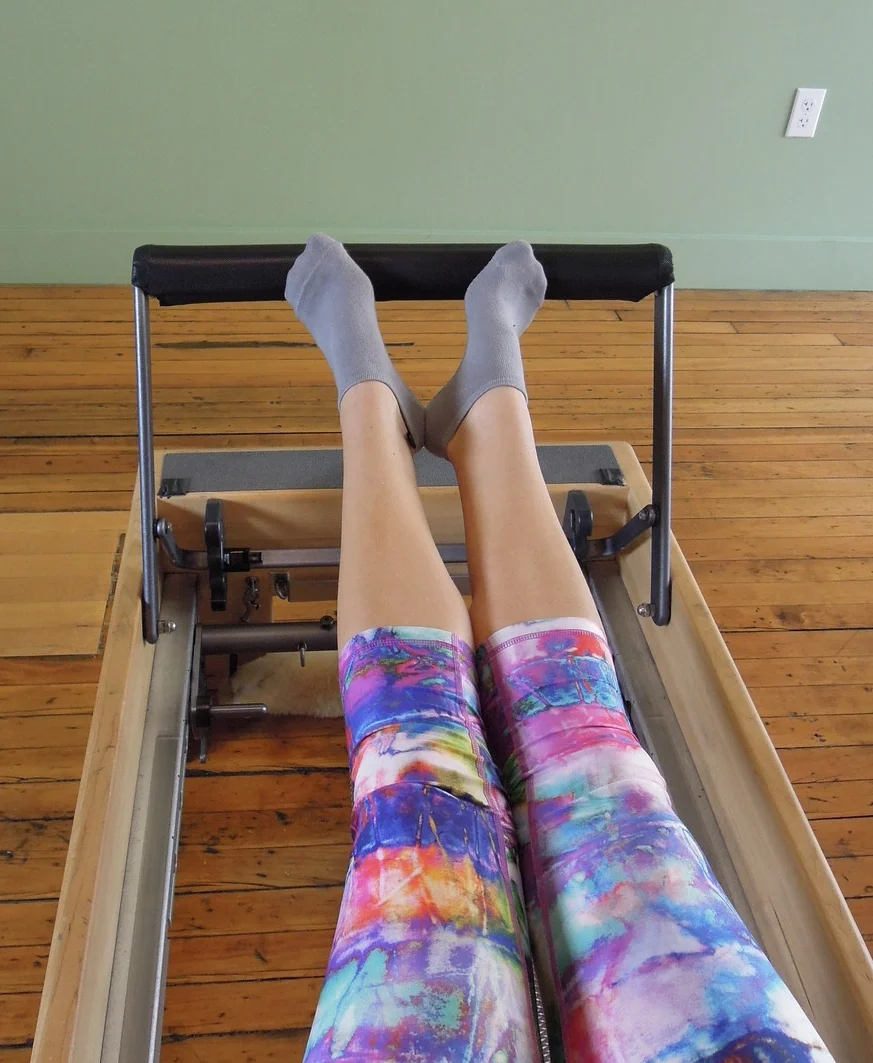












WHAT EXERCISES REDUCE TFL PAIN & TIGHTNESS?





Conclusion
There are six different degrees of movement at the hip joint (flexion, extension, abduction, adduction, internal rotation, and external rotation). Familiarise yourself with clinical anatomy and which muscles work through which range and movement. Educate your clients on where they should be driving the control from and maybe try these teaching cues to improve their technique.
The TFL is such a little muscle, poor thing, it can be so painful when overloaded. Boss & Connell (2002) investigate the size of TFL and noted that the average size of TFL is 2.1mm thick and 18cm long! Thats not a very big muscle for producing force.
Let's help it out a bit by bringing up the primary muscles and correcting movement patterns. Hope this gives everyone some ideas to try in-rooms, in a gym setting, pilates setting, and never forget all the great independent home-based exercises.
Sian
References
Antonio, S., Wolfgang, G., Robert, H., Fullerton, B., & Carla, S. (2013). The anatomical and functional relation between gluteus maximus and fascia lata.Journal of bodywork and movement therapies, 17(4), 512-517.
Bass, C., & Connell, D. (2002). Sonographic findings of tensor fascia lata tendinopathy: another cause of anterior groin pain. Skeletal radiology, 31(3), 143-148.
do Carmo Carvalhais, V. O., de Melo Ocarino, J., Araújo, V. L., Souza, T. R., Silva, P. L. P., & Fonseca, S. T. (2013). Myofascial force transmission between the latissimus dorsi and gluteus maximus muscles: an in vivo experiment.Journal of biomechanics, 46(5), 1003-1007
Grimaldi, A., Richardson, C., Durbridge, G., Donnelly, W., Darnell, R., & Hides, J. (2009). The association between degenerative hip joint pathology and size of the gluteus maximus and tensor fascia lata muscles. Manual therapy, 14(6), 611-617.
Lee, J. H., Cynn, H. S., Kwon, O. Y., Yi, C. H., Yoon, T. L., Choi, W. J., & Choi, S. A. (2014). Different hip rotations influence hip abductor muscles activity during isometric side-lying hip abduction in subjects with gluteus medius weakness. Journal of Electromyography and Kinesiology, 24(2), 318-324.
Selkowitz, D. M., Beneck, G. J., & Powers, C. M. (2013). Which exercises target the gluteal muscles while minimizing activation of the tensor fascia lata? Electromyographic assessment using fine-wire electrodes. journal of orthopaedic & sports physical therapy, 43(2), 54-64.
Sidorkewicz, N., Cambridge, E. D., & McGill, S. M. (2014). Examining the effects of altering hip orientation on gluteus medius and tensor fascae latae interplay during common non-weight-bearing hip rehabilitation exercises.Clinical Biomechanics, 29(9), 971-976.
Sutter, R., Kalberer, F., Binkert, C. A., Graf, N., Pfirrmann, C. W., & Gutzeit, A. (2013). Abductor tendon tears are associated with hypertrophy of the tensor fasciae latae muscle. Skeletal radiology, 42(5), 627-633.

