Treatment Strategies for Cervicogenic Dizziness
This is the fourth (and final) sequel to three previous blogs on sensorimotor dysfunction, the distinguishing features of cervicogenic dizziness, and differential diagnosis of CGD, this blog aims to explore the treatment strategies for CGD.
For treatment to be effective it needs to be specifically targeted to impairments in the cervical spine, vestibular system and sensorimotor system. Our role as physiotherapists’ is to accurately identify red flags and to choose which cases will benefit from physiotherapy management.
A RECAP OF THE EXAMINATION
To read in further detail about the subjective and physical examination click on the links below to previous blogs on this topic.
- What words best describe your dizziness/unsteadiness?
- How often do you get these symptoms?
- How long do they last?
- What brings on these symptoms?
- When you experience these symptoms what do you do?
- Have you fallen or lost balance when these symptoms occur?
- Is there anything else that occurs at the same time?
- How soon after the accident did these symptoms occur?
- Neurological examination (CNS) adding coordination testing, ataxia testing, upper motor neurone assessment, reflexes, sensation, manual muscle testing. Looking for dysmetira, dysdiadokinesis, rigidity (ruling out other causes of dizziness).
- Cervical spine examination – AROM, PROM, manual palpation, muscle length tests, and DCNF strength.
- Vestibular assessment & Sensorimotor assessment includes the rhomberg’s test (balance), hall-pike dix manouevre (BPPV), gaze stability, smooth pursuit, head thrust test, and joint position error test.
What dysfunctions can we expect to find?
Joint Position Error (optokinetic system).
Treleaven, et al. (2003) found that joint position error (JPE) is significantly greater in whiplash associated disorders than in healthy controls. JPE is related to altered cervical mechanoreceptor function. This reduced proprioception often leads to over-shooting of movement. In particular, the authors revealed that in WAD large amounts of JPE, particularly in rotation, are more prevalent in those who suffer from dizziness.
Gaze stability and smooth pursuit neck torsion (oculomotor system).
In 2004, Treleaven, Jull and Choy investigate the presence of deficits in gaze stability and smooth pursuit neck torsion in relation to WAD and dizziness. Their results found that deficits in SPNT test are present more in patients with WAD, compared to healthy controls, and more prevalent in those who reported dizziness and unsteadiness.
Balance.
The third study explored the balance disturbances in WAD compared to healthy controls using the balance error scoring system (BESS). Their results indicated that when compared to health subjects, patients with WAD have significant deficits in standing balance beyond the first level (feet apart, eyes open, firm surface), and that performance was most impaired in those with higher levels of reported dizziness and neck pain (Treleaven, et al., 2005).
Neck pain.
Compare to balance disturbances and sensorimotor dysfunction, neck pain is the least specific measure of dysfunction in CGH. Treleaven, et al. (2011) conducted a fourth study looking a the correlation between neck pain and WAD and dizziness and were unable to draw strong conclusions that neck pain correlates with high levels of sensorimotor dysfunction. This emphasises to the reader that neck pain, although it may be upper cervical in origin, is not a sufficient measurement of sensorimotor dysfunction and that a thorough assessment of each element of postural stability is required.
Vestibular dysfunction.
Unlike BPPV and other causes of vertigo, cervicogenic dizziness may have a component of vestibular dysfunction due to the multi-direction impact on cervical afferents (VCR) and occular afferents (VOR). Therefore, vestibular rehabilitation exercises may be used to retrain gaze stability, balance and maintenance of neck position and postural stability.
Targeted intervention
Many articles have since been published exploring physiotherapy management of WAD, which now includes rehabilitation of:
- The cervical spine
- Vestibular and balance rehabilitation
- Joint position sense
- Gaze stability and smooth pursuit retraining
- Exercise therapy
The findings of these studies is helpful to us as Physiotherapists because they provide information on how best to treat a patient with multiple dysfunctions, one of them being disruption in somatosensory function resulting in cervicogenic dizziness.
There is no set treatment approach for cervicogenic dizziness just as there is no gold standard assessment for diagnosis. We need to assess all systems above and then use the "treat what you find" approach. Here are some of the ways we can approach the cervical, vestibular and sensorimotor impairments found to be associated with cervicogenic dizziness.
Manual therapy of the cervical spine
The first and most common choice of treatment is manual therapy. As sensorimotor dysfunction is often linked to dysfunction in movement and control of the cervical spine, it seems only logical that we need to treat the cervical spine to restore movement, strength and function. A systematic review of the literature noted that all studies of manual therapy treatment of patients with cervicogenic dizziness reported consistent post-treatment decreases in symptoms and signs of dizziness (Schenk, et al., 2006. P.E58). As the diagnosis of cervicogenic dizziness is one of exclusion, there still seems to be a lack on high quality studies exploring the treatment effectiveness. None-the-less, below are some recommendations from the studies I read.
Manual therapy treatments which may be effective are ones that focus on:
- Improving neck range of movement,
- Reducing neck pain,
- Improving muscle strength and postural control, and
- Reducing tenderness on palpation.
Techniques worth exploring may include soft tissue techniques, Maitland mobilisations (PAIVMS and PPIVMS), Mulligan's SNAGs and NAGs, and manipulation.
There was one study by Reid, et al., (2012) exploring the treatment effectiveness of Mulligan Sustained Natural Apophyseal Glides (SNAGs) compared to Maitland passive joint mobilisation compared to a control group in the reduction of symptoms of cervicogenic dizziness. Unfortunately this study had no standardised treatment protocol and the treatment dosage (between 2-6 treatments over 6 weeks) was left to the physiotherapists’ discretion, which limits the generalisability and external validity of this study.
The general guidelines each therapist followed for performing a SNAG was an upslope glide on C1 or C2 in the direction of rotation restriction repeated 6 times in the first session and up to 10 times in subsequent sessions. The aim was to perform treatment without provoking dizziness. PAIVMs were performed 3 x 30 seconds on the most painful upper cervical joints determined by manual palpation during the assessment. What we take away from this study is that sticking to the treatment principles for performing a treatment (such as Maitland mobilisations) is the best approach for managing joint stiffness, pain and limited range, as apposed to following a treatment recommendation/recipe based on the research trials.
Vestibular rehabilitation
"Vestibular rehabilitation is sometimes a necessary adjunct to the treatment of patients with dizziness of suspected cervical origin. Several authors have reported successful outcomes when incorporating vestibular rehabilitation exercises with OMPT in the treatment of patients with cervicogenic dizziness” (Schenk, et al., 2006, p. E58). There is a lack of strong evidence supporting the combination of vestibular rehabilitation and manual therapy over manual therapy alone so clinically you'll need to evaluate the benefits for each individual client and determine how much of the dizziness is related to vestibular over cervical dysfunction (Lystad, et al., 2011).
Balance training can be as simple or complex as the patient requires. The aim is not to provoke their dizziness while still developing a stronger sense of balance. A great starting point is to practice the position they could complete successfully during the Rhomberg's test or BESS. The aim is to sustain balance for 30 seconds before moving to a more complicated task.
Begin with a supportive surface before moving to a foam block, trampoline or wobble board. Feet together, tandem stance and single leg stance are all great positions for retraining balance. If you're wanting to get even more complicated you can superimpose joint position sense exercises or oculomotor and optokinetic training on top of the balance exercises.
Joint position sense (sensorimotor training)
After completing your assessment of sensory motor function you can design exercises around the impairments you identified. When designing exercises for sensorimotor function they should not provoke dizziness and therefore they can be started within the first or second treatment session (Sterling, et al., 2008, p. 223).
Training joint position sense is achieved through relocation tasks. While rotation is the most commonly demonstrated movement you might see, all directions of cervical movement should be retraining for joint position sense. Essentially you are going to begin in sitting (with good posture) and turn to the head to one side and then return to centre. Using the lazer head band for visual feedback is a great learning tool. Patient's should be positioned 1m away from the wall to do the exercises. To progress joint position sense exercises you can change posture to standing, perform exercises with eyes closed or get the patient to follow a moving object.
Gaze stability & Smooth pursuit (sensorimotor training)
A major benefit of some of these exercises is that they can be performed even when the patient has restrictions in neck movement due to pain or articular dysfunction, particularly the smooth pursuit movements. The exercises can be performed until some dizziness is provoked but not neck pain should be reproduced (Sterling, et al., 2008, chpt 14).
The first goal is to train eye-following movements. Generally these exercise begin in sitting but if needed, the patient can be positioned in lying for more support. These photos show lateral eye movements but remember that you want to train all directions of movement i.e up/down, left/right, circular and diagonal movements. In terms of dosage you can commence at 5-10 second bursts and build to 30 seconds, performed as frequently as 5 times a day (Sterling, et al., 2008, p. 225).
To progress these exercises you can change position (sitting to standing), trunk rotation (to mimic the smooth pursuit test) and speed of movement.
The next stage of exercises involve gaze fixation with head movements. The pictures below show a starting level for these exercises. They can be progressed into standing, walking, by increasing speed, by restricting peripheral vision or by making the background behind the object complex.
A great example of functional progression is asking your patient to walk down a busy shopping isle while fixating on a specific object on the shelf. Interestingly, the first patient I ever treated for cervicogenic dizziness described how her major trigger for dizziness was doing the weekly shopping. She felt so dizzy walking down the isles that she relied on her shopping trolley for balance. The her husband started accompanying her to the store and when he decided to push the trolley she soon found the dizziness unbearable.
The final stage of oculomotor training involves eye-head coordination in which the eyes and head move together in the same direction. From there the exercise can be progressed so that the eyes move first and then the head follows. Once this coordination is established you can move eyes and head between two fixed objects. The final progression is moving the eyes and head in opposite directions.
Exercise therapy
When it comes to exercise therapy there are a few principles to follow (Sterling, et al., 2008, chpt 14):
- Commence the exercises early in treatment.
- Exercises should not provoke neck pain.
- Exercises should be taught and performed precisely and specifically target muscular control and sensorimotor dysfunction.
- Exercises need to be functionally specific and patients should be education on their importance in rehab if compliance is going to be established.
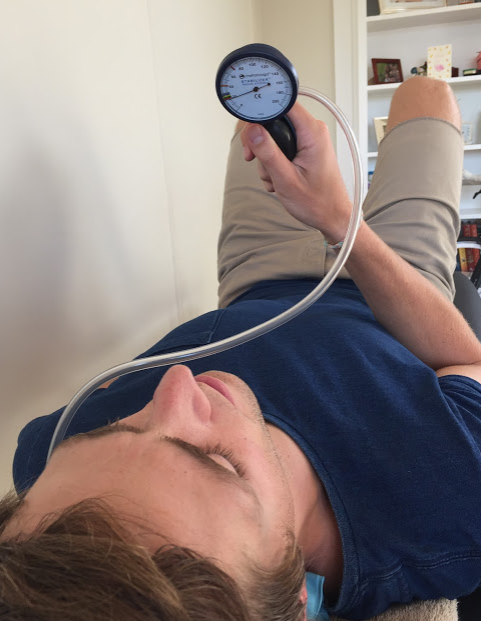
The first phase in muscular training is to teach patients how to activate the deep stabilising muscles. A great place to start in this phase is by using the pressure biofeedback unit for education and teaching of technique. The aim is to develop technique and low load endurance before integrating these muscles into more functionally-specific exercises (Sterling, et al., 2008, chpt 14). The stages of retraining the cervical muscular system is much more involved that just deep cervical neck flexion exercises and involve the extensor muscles too. These phases of rehabilitation will be addressed separately. For now, remember that it is a safe and useful place to begin your rehabilitation for patients with muscular and postural impairments associated with cervicogenic dizziness.
Summary
As the research continues to develop so will our understanding of the neurophysiological mechanisms underlying persistent neck pain, dizziness and unsteadiness in both cervicogenic dizziness and dizziness associated with whiplash. Identifying deficits in sensorimotor function is only the beginning of a new approach to manage of WAD and cervicogenic dizziness, as we discover more about the dysfunction in cervical afferent function.
In order for our interventions to accurately target the contributing impairments involved in dizziness we need to carefully assess neurological function, the cervical spine and sensorimotor dysfunction. While neck pain may be present in patients with cervicogenic dizziness, it is the impairments in oculomotor system, optokinetic system and balance systems that help distinguish this type of dizziness from true vertigo, BPPV and other conditions. Treatments that collectively target these impairments are likely to have the most positive outcomes in patient improvement.
Next time a patient presents with dizziness my hope is that you feel more equipped with knowledge:
- About the possible causes of dizziness,
- How to conduct a thorough subjective and objective examination, and
- If the cervical spine is suspected as the source of dizziness, how to manage cervical, vestibular and sensorimotor which contribute cervicogenic dizziness.
At the start of research this topic I couldn't even define what sensorimotor dysfunction was and had little knowledge about how it is related to cervicogenic dizziness. Coming to the end of this blog series on sensorimotor dysfunction and cervicogenic dizziness I feel like I've learnt something in each of the dot points above. For further information about treatment of cervicogenic dizziness and with particular respect to whiplash associated disorders my preferred reference is Whiplash, headache, and neck pain: research-based directions for physical therapies, which I've highlighted in the reference list below.
Sian :)
References:
Dispenza, F., De Stefano, A., Mathur, N., Croce, A., & Gallina, S. (2011). Benign paroxysmal positional vertigo following whiplash injury: a myth or a reality? American journal of otolaryngology, 32(5), 376-380.
Lystad, R. P., Bell, G., Martin, B. S., & Carter, C. V. (2011). Manual therapy with and without vestibular rehabilitation for cervicogenic dizziness: a systematic review. Chiropractic & Manual Therapies, 19(1), 21.
Reid, S., & Rivett, D. (2005). Manual therapy treatment of cervicogenic dizziness: a systematic review. Manual therapy, 10(1), 4-13.
Reid, S., Rivett, D., Katekar, M., & Callister, R. (2008). Sustained natural apophyseal glides (SNAGs) are an effective treatment for cervicogenic dizziness. Manual therapy, 13(4), 357-366.
Reid, S., Rivett, D., Katekar, M., & Callister, R. (2012). Efficacy of manual therapy treatments for people with cervicogenic dizziness and pain: protocol of a randomised controlled trial. BMC musculoskeletal disorders, 13, 201-209.
Schenk, R., Coons, L. B., Bennett, S. E., & Huijbregts, P. A. (2006). Cervicogenic dizziness: A case report illustrating orthopaedic manual and vestibular physical therapy comanagement. The Journal of manual & manipulative therapy, 14(3), E56-E68.
Sterling, M., Falla, D., Jull, G., Treleaven, J., & O'Leary, S. (2008). Whiplash, headache, and neck pain: research-based directions for physical therapies: Elsevier Health Sciences.
Treleaven, J., Clamaron Cheers, C., & Jull, G. (2011). Does the region of pain influence the presence of sensorimotor disturbances in neck pain disorders? Manual therapy, 16(6), 636-640.
Treleaven, J., Jull, G., & Low Choy, N. (2004). Smooth pursuit neck torsion test in whiplash-‐associated disorders: relationship to self-reports of neck pain and disability, dizziness and anxiety. Journal of rehabilitation medicine, 37(4), 1-1.
Treleaven, J., Jull, G., & Low Choy, N. (2005). Standing balance in persistent whiplash: a comparison between subjects with and without dizziness. Journal of rehabilitation medicine, 37(4), 224-229.
Treleaven, J., Jull, G., & Sterling, M. (2003). Dizziness and unsteadiness following whiplash injury: characteristic features and relationship with cervical joint position error. Journal of rehabilitation medicine, 35(1), 36-43.